Food Accessibility, Insecurity and Health Outcomes
Having access to nutritious food is a basic human need.
- Food security means having access to enough food for an active, healthy life.
- Nutrition security means consistent access, availability, and affordability of foods and beverages that promote well-being, prevent disease, and, if needed, treat disease.
On the other hand, food and nutrition insecurity is an individual-, household-, and neighborhood-level economic and social condition describing limited or uncertain access to adequate and affordable nutritious foods and is a major public health concern.
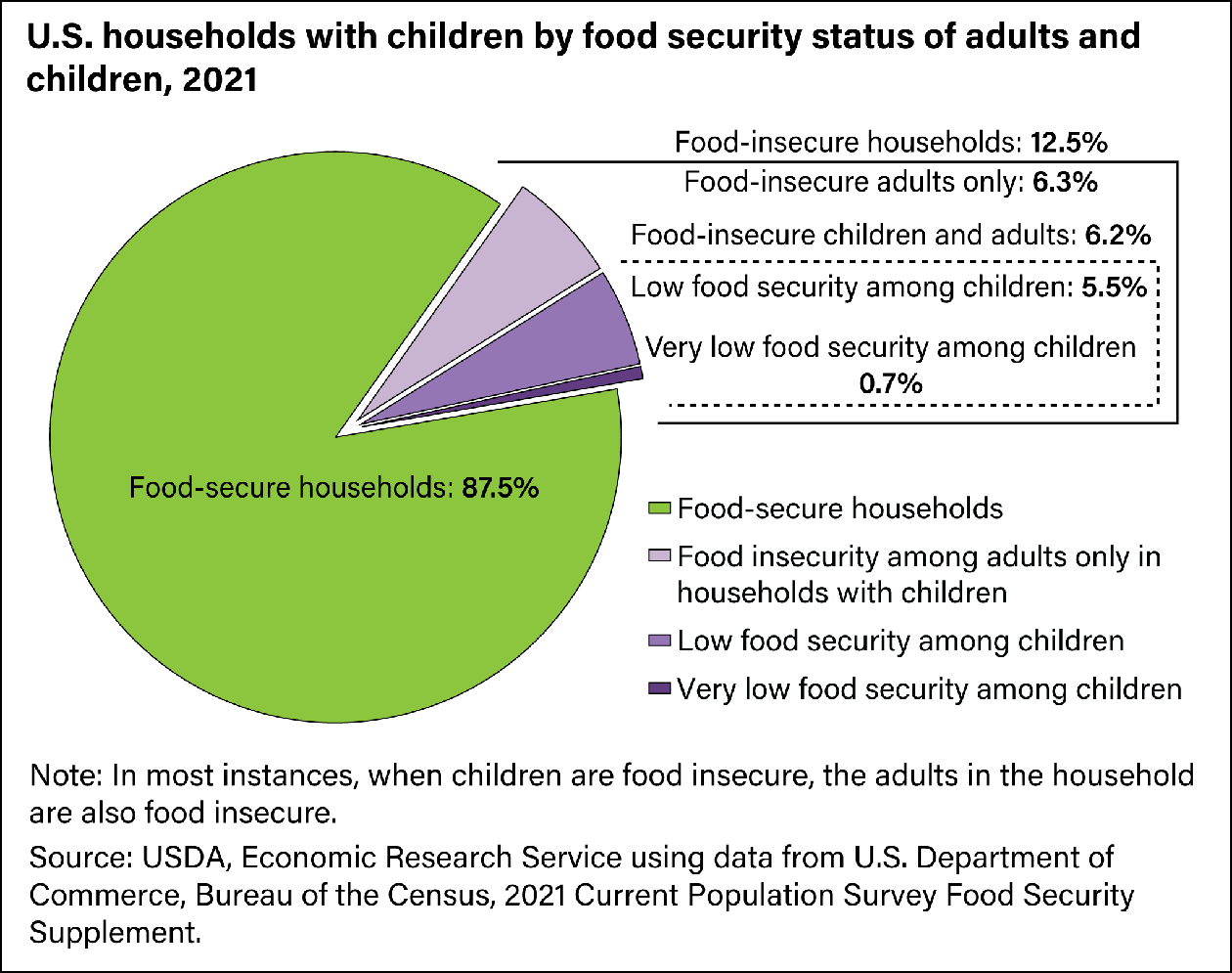
Food insecurity and the lack of access to affordable nutritious food are associated with increased risk for multiple chronic health conditions such as diabetes, obesity, heart disease, mental health disorders and other chronic diseases. In 2020, almost 15% of U.S. households were considered food insecure at some point in time, meaning not all household members were able to access enough food to support active, healthy lifestyles. In nearly half of these households, children were also food insecure (see chart above), which has implications for human development and school experience. Food insecurity disproportionately affects persons from racial and ethnic minority and socioeconomically disadvantaged populations:
- 20% of Black/African American households were food insecure at some point in 2021, as were 16% of Hispanic/Latino households when compared to 7% of White households.
- Food insecurity for U.S. Hispanic/Latino adults differs by origin. Current national data is not available but from 2011-2014 food insecurity was highest among those identifying from Puerto Rico (25.3%), followed by Mexico (20.8%) Central and South America (20.7%) and Cuba (12.1%).
- In the past 20 years, American Indian/Alaskan Native (AI/AN) households have also been at least twice as likely to have experienced food insecurity when compared with White households, often exceeding rates of 25% across different regions and AI/AN communities.
- Native Hawaiian and Pacific Islander (NHPI) adults also experience a high food insecurity prevalence (20.5%) and had significantly higher odds of experiencing low and very low food security compared with White households.
- While national data on specific Asian American national origin populations is not readily available, among Asian Americans living in California from 2001-2012, food insecurity was highest among Vietnamese households (16.4%), followed by Filipino (8.3%), Chinese (7.6%), Korean (6.7%), South Asian (3.14%), and Japanese households (2.3%), highlighting considerable variation across Asian American communities.
- Food insecurity is inextricably linked to poverty, with 35.3 % of households with incomes below the federal poverty line being food insecure.
- Although the graph below on national trends in food insecurity does not capture the full impact of the COVID-19 pandemic, food insecurity is likely to increase, and racial and ethnic disparities in food insecurity experiences could worsen.
Healthy food accessibility and insecurity is a social determinant of health.
Food and nutrition insecurity are predominantly influenced by the local environment, including surrounding neighborhood infrastructure, accessibility, and affordability barriers. Access to grocery stores that carry healthy food options (such as fresh fruit, vegetables, low-fat fish and poultry) are not located equitably across residential and regional areas in the United States.
Areas that lack access to affordable, healthy foods are known as food deserts. Food deserts are:
- Found in urban or suburban neighborhoods that lack grocery stores (supermarkets or small grocery stores) that offer healthy food options.
- Found in rural areas and neighborhoods where the nearest grocery stores are too far away to be convenient or accessible.
- More prevalent in neighborhoods that are comprised of a majority of racial or ethnic minority residents or in rural AI/AN communities.
- More likely found in areas with a higher percentage of residents experiencing poverty, regardless of urban or rural designation.
Urban, suburban, and rural areas can also be overwhelmed with stores that sell unhealthy calorie-dense and inexpensive junk foods, including soda, snacks, and other high sugar foods. This is known as a food swamp. Food swamps:
- Reduce access to nutritional foods and provide easier access to unhealthy foods.
- Are a predictor of obesity, particularly in communities where residents have limited access to their own or public transportation and experience the greatest income inequality.
Reducing food and nutrition insecurity in the U.S. will require a multifaceted approach that considers, among other possibilities:
- Strategies that engage communities in local health programs; for example, recruiting community partners to assist in addressing gaps between food access and intake.
- Interventions that utilize federal food and nutritional supplemental programs, including the Supplemental Nutrition Assistance Program (SNAP) and the Special Supplemental Nutritional Program for Women, Infants, and Children (WIC).
- Leveraging local and federal policies targeting food insecurity; for example, retail store interventions, where healthy food placement, promotion and price influence healthier choices; sweetened beverage taxes to reduce the purchase appeal to consumers; and junk food taxes balanced with removal of taxes on water and fruits and vegetables.
NIMHD is studying and addressing issues related to food and nutrition insecurity through a variety of initiatives:
NIH Publication
Research Opportunities to Address Nutrition Insecurity and Disparities
Coauthored by Shannon N. Zenk, Lawrence A. Tabak and Eliseo J. Pérez-Stable, JAMA 2022
NIMHD Events on Food Insecurity
Food Insecurity, Neighborhood Food Environment, and Nutrition Health Disparities: State of the Science
NIMHD co-sponsored this September 2021 workshop led by the NIH Office of Nutrition Research and its Nutrition and Health Disparities Implementation Working Group
NIMHD Hosts Senior Research Investigators to Present on Food Insecurity and Related Topics:
NIMHD co-sponsored the November 2020 virtual workshop NIH Rural Health Seminar: Challenges in the Era of COVID-19. This workshop focused on long-standing health disparities and social inequities experienced by rural populations, and featured experts on food insecurity, including:
- Dr. Brenda Eskenazi, Professor in Maternal and Child Health and Epidemiology, Brian and Jennifer Maxwell Endowed Chair in Public Health and Director of the Center for Environmental Research and Children’s Health, University of California, Berkeley, who spoke on the topic of COVID-19 and the impact on health of Californian farmworkers.
- Dr. Alice Ammerman, Mildred Kaufman Distinguished Professor of Nutrition, Director, Center for Health Promotion and Disease Prevention, University of North Carolina, who spoke on interventions to address job loss and food security in rural communities during COVID.
NIMHD Content on Food Insecurity
NIMHD Science Visioning and Research Strategies
As part of the Scientific Visioning Research Process, NIMHD developed a set of 30 strategies to transform minority health and health disparities research. Several of these strategies focus on issues related to food security and accessibility, including:
- Assessing how environment and neighborhood structures such as areas where people have limited access to a variety of healthy and affordable foods (or food deserts) influence health behaviors.
- Promoting multi-sectoral interventions that address the structural drivers of food deserts.
- Promoting interventions that address the social determinants of health within health care systems, including food insecurity.
Publications
Food Insecurity and Obesity: Research Gaps, Opportunities, and Challenges
Dr. Derrick Tabor, NIMHD Program Officer, co-authored “Food insecurity and obesity: research gaps, opportunities” in Translational Behavioral Medicine. This review highlights NIH funding for grants related to food insecurity and obesity, identifies research gaps, and presents upcoming research opportunities to better understand the health impact of food insecurity.
NIMHD Research Framework
Native Hawaiian Health Adaptation
The NIMHD Research Framework was adapted by Keawe’aimoku Kaholokula, Ph.D., University of Hawai’i at Mānoa, to reflect social and cultural influences of Native Hawaiian health. Ka Mālama Nohona (nurturing environments) to support Native Hawaiian health include strategic goals of food sovereignty and security to promote a strong foundation for healthy living.
NIMHD Articles
- The Osage Community Supported Agriculture Program: A Tribal Nation’s Effort Toward Food Security and Food Sovereignty
- The Navajo Nation Junk Food Tax and the Path to Food Sovereignty
- Fighting Cancer—and Reducing Disparities—Through Food Policy
- Fresh Food for the Osage Nation: Researchers and a Native Community Work Toward Improved Food Resources and Food Sovereignty
- Amplifying the Voice of Native Hawaiian and Pacific Islander Communities Amid the COVID-19 Crisis by Joseph Keawe‘aimoku Kaholokula, Ph.D.
- Racism and the Health of Every American by NIMHD Director Eliseo J. Pérez-Stable, M.D.
- The Future of Minority Health and Health Disparities Research by Tany Agurs-Collins, Ph.D., R.D., and Susan Persky, Ph.D.
- Addressing Social Needs and Structural Inequities to Reduce Health Disparities: A Call to Action for Asian American and Pacific Islander Heritage Month by Marshall H. Chin, M.D., M.P.H.
- “Insights” on Simulation Modeling and Systems Science, New Research Funding Opportunity by Xinzhi Zhang, M.D., Ph.D.
NIMHD Funding Resources and Opportunities
Funding Opportunity Announcements (FOAs)
NIMHD supports many FOAs that include topics related to food security as an area of research interest:
- Request for Information: Food Is Medicine Research Opportunities
- Notice of Special Interest: Stimulating Research to Understand and Address Hunger, Food and Nutrition Insecurity
- Community Level Interventions to Improve Minority Health and Reduce Health Disparities (R01 Clinical Trial Optional)
- Addressing Health Disparities Among Immigrant Populations through Effective Interventions (R01 Clinical Trial Optional)
- Health Services Research on Minority Health and Health Disparities (R01 Clinical Trial Optional)
- Long-Term Effects of Disasters on Health Care Systems Serving Populations Experiencing Health Disparities (R01 Clinical Trial Optional)
- Please see our list of Active NIMHD Funding Opportunities for more.
NIMHD-Supported Research Projects
See a list of active NIMHD-supported research projects studying food security and related topics.
NIMHD-Supported, NIH-Wide Initiatives
The PhenX Toolkit provides recommended and established data collection protocols for conducting biomedical research. There are PhenX protocols available for assessing and understanding food insecurity and food swamps.
The Strategic Plan for NIH Nutrition Research is the first NIH-wide strategic plan for nutrition research that highlights crosscutting, innovative opportunities to advance nutrition research from basic science to experimental design to research training. The plan emphasizes the need for studies on minority health and nutrition-related health disparities research.
Additional Resources and Data
The Centers for Disease Control’s Healthier Food Environments: Improving Access to Healthier Foods discusses CDC efforts to improve food access within the community.
The United States Department of Agriculture has two databases that compile national data on food accessibility:
- The Food Access Research Atlas provides food access data for populations within census tracts and mapped overviews of food access for low-income communities.
- The Food Environment Atlas assembles statistics on food environment indicators to stimulate research on the determinants of food choice and diet quality.
The Healthy People initiative provides 10-year, measurable public health objectives and useful tools to help track progress. The Healthy People 2030 includes food insecurity as a social determinant of health.
Page updated July 3, 2024